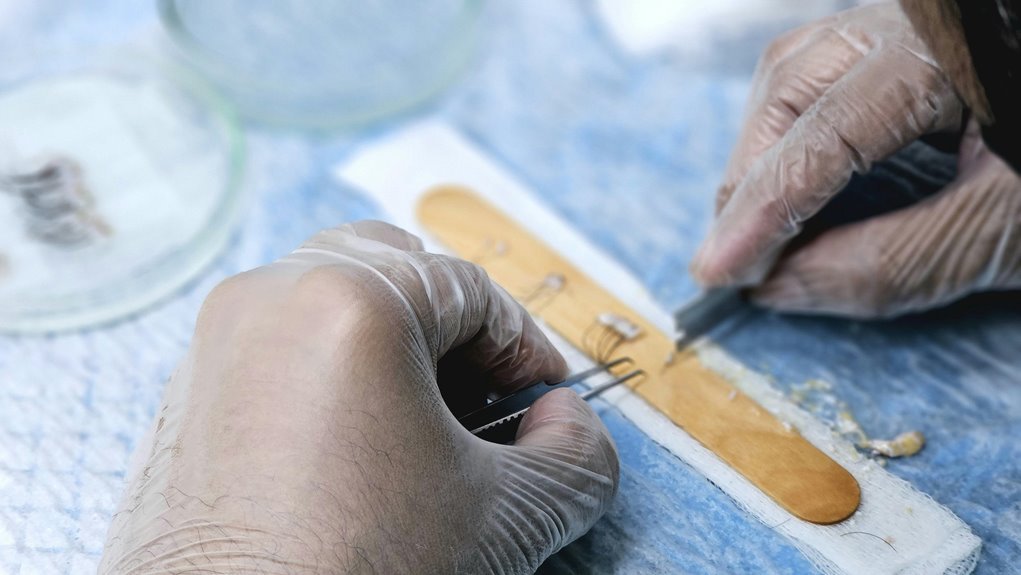
A medical registry focused on heart transplantation clarifies its scope by explicitly omitting broader cardiovascular transplant data. It emphasizes alerts and logs as frontline, timestamped streams that feed clinical dashboards for rapid triage of post-transplant complications. Governance is designed to safeguard data integrity and reproducibility, supporting trajectory analyses and cross-center benchmarking. Yet critical gaps remain in mapping transplant pathways, raising questions about how these elements will integrate with policy and multi-center research—stability hinges on disciplined, extensible design.
What a Medical Registry Overview Lacks Without Heart Transplant Data
One key limitation of a Medical Registry Overview that omits heart transplant data is the potential misalignment between general cardiovascular outcomes and transplant-specific trajectories, which can obscure the true scope and quality of patient care.
This absence highlights data gaps, complicating interpretation, limiting targeted improvements, and reducing capacity to benchmark heart transplant pathways against broader, non-transplant cardiovascular benchmarks with precision.
How Alerts and Logs Drive Early Complication Detection
Alerts and logs function as the frontline data streams that enable near-instantaneous recognition of post-transplant complications. They provide continuous, timestamped input to clinical dashboards, supporting rapid triage and intervention.
Systematic analysis reveals how alert latency can shape response times, while data governance ensures integrity, traceability, and reproducibility across care teams and monitoring platforms, enhancing overall patient safety and outcomes.
Designing a Registry: Data Points, Privacy, and Audit Trails
Registry design for heart transplantation hinges on selecting data points that balance clinical utility with feasibility. The design emphasizes data elements, privacy safeguards, and clear audit trails, enabling accountability without overreach. Troubleshooting governance frameworks ensure compliance and rapid issue resolution. Interoperability standards guide data exchange, supporting consistent definitions across systems while preserving patient confidentiality and facilitating scalable, analyzable registry operations.
Using the Registry for Outcomes Improvement and Research
To improve patient outcomes and advance scientific understanding, the registry is leveraged to quantify post-transplant trajectories, identify patterns of graft function, rejection, and complications, and benchmark performance across centers.
Outcomes research supports improved patient stratification and hypothesis generation, enabling standardized comparisons.
The approach fosters cross border collaboration, accelerates evidence generation, and informs policy, guidelines, and resource allocation for continuous quality improvement.
Conclusion
This registry, while focused on heart transplantation, demonstrates that narrowly scoped data can still illuminate broader care trajectories when coupled with precise alerts and auditable logs. The central theory—that targeted transplant pathways catalyze cross-domain insights—holds true, provided governance preserves data integrity and reproducibility. A systematic synthesis of timely complication signals and longitudinal outcomes enables benchmarking and policy refinement. Future work should expand cross-center collaboration to validate findings and accelerate evidence-based improvements in transplant ecosystems.